Blog
Kids, sugar and the liver
 Incidence of non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH) is increasing.
Incidence of non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH) is increasing.
NAFLD is the build-up of excess fat in liver cells and often associated with insulin resistance, overweight, and high blood triglycerides.1
NASH can be considered the more extreme end of the NAFLD spectrum, where severe inflammation can lead to irreversible damage, fibrosis, and cirrhosis of the liver.2-3
Liver fat accumulation impacts effective liver function.
Why does this matter?
Among a myriad of other roles, the liver is one of the major detoxifying organs of the body, processing various compounds from the internal and external environment to be either expelled or recycled for future use.
Fatty liver is usually caused by drinking too much booze. Now, due to other dietary factors such as excess free and added sugar, we are seeing people who are not large consumers of alcohol with fatty livers. It is now the fastest growing cause of liver disease in the Western world. Even in kids.4
A study from Italy shared startling results on the independent link between obese children and adolescents with NAFLD, and fructose consumption, uric acids levels, and incidence of NASH.5
Diet records were taken from 271 participants, with an average age of 12.5 years. The researchers found the greatest source of fructose was sugar-sweetened beverages, and 90% of these kids consumed a soft or sweetened drink at least once per week.
Then the researchers measured the incidence of NASH.
Shockingly, 37.6% of patients had NASH. Of those with NASH, 47% had high uric acid, compared to only 29.7% of non-NASH participants.
Uric acid in high concentrations can crystallise, causing pain and the condition known as gout.
After adjusting for multiple confounding factors, uric acid levels and free fructose consumption were each independently and positively associated with NASH. The researchers also found the only independent dietary risk factor for increased uric acid in the blood was free fructose consumption.
“In the intestine, fructose intake alters the gut microbiome and enhances endotoxin translocation into the portal circulation via increased permeability of tight junctions. In the liver, fructose is rapidly metabolized, consuming adenosine triphosphate, which may result in increased adenosine monophosphate and inosine monophosphate (IMP) and conversion of IMP to uric acid,” the researchers wrote.
It is important to remember that free and added sugars are the concern when discussing excessive fructose intake – not the fructose naturally occurring in whole foods like fruit. Sugars in fruit are packaged and delivered to the body alongside beneficial fibre, minerals, vitamins, and phytonutrients, altering the way it is digested and absorbed by (and therefore its impact on) the body.
Understanding the metabolic effects excess free sugar consumption has on our kids and teens is important, especially as some kids are consuming far too much.
“The development of NASH may markedly affect life expectancy and quality of life in affected individuals and therefore it is crucial to understand the risk factors for NASH in children and adolescents in order to design effective interventions which can be used safely to treat this young group of patients,” said study author Valerio Nobili.
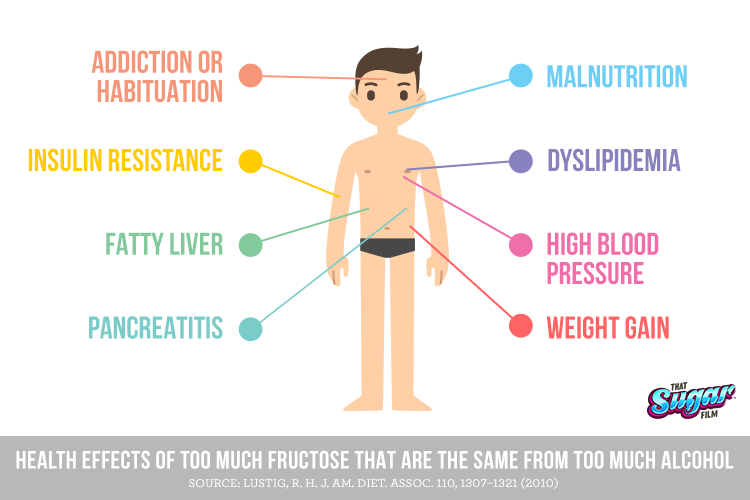
Pediatric Endocrinologist Prof. Robert Lustig published an article several years back, likening the effects of ethanol (alcohol) and excess free fructose (and it is not limited to the liver).6
Unfortunately, it is currently predicted the incidence of fatty liver in Australia will increase by 25%, by 2030, largely due to childhood obesity and the consumption of sugary drinks.7-8
Education is critical for our kids to understand the short and long-term implications of consuming too much discretionary food in place of the real stuff, and how to identify the added sugars in seemingly healthy foods.
Not sure where to start? Check out our sugary swaps for kids!
So, love the liver and go easy on the sweet stuff, especially sugary drinks.
By Angela Johnson (BHSc Nut. Med.)
References:
- Better Health Channel 2012, Liver- fatty liver disease, viewed 15 February 2017, <https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/liver-fatty-liver-disease>.
- Cleveland Clinic 2013, Nonalcoholic fatty liver disease, viewed 15 February 2017, <http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/hepatology/nonalcoholic-fatty-liver-disease/>.
- Dyson, JK, Anstee, QM, & McPherson, S 2014, ‘Non-alcoholic fatty liver disease: a practical approach to diagnosis and staging’, Frontline Gastroenterology, vol. 5, no. 3, pp. 211-218.
- Bellentani, S, Scaglioni, F, Marino, M, & Bedogni, G 2010, ‘Epidemiology of non-alcoholic fatty liver disease’, Digestive Diseases (Basel, Switzerland), vol. 28, no. 1, pp. 155-161.
- Mosca, A et al. 2017, ‘Serum uric acid concentrations and fructose consumption are independently associated with NASH in children and adolescents’, Journal of Hepatology, [ePub ahead of print].
- Lustig, RH 2010, ‘Fructose: Metabolic, Hedonic, and Societal Parallels with Ethanol’, Journal of the American Dietetic Association, no. 9, p. 1307.
- Adams, LA et al. 2020, ‘Nonalcoholic fatty liver disease burden: Australia, 2019–2030’, Journal of Gastroenterology and Hepatology, https://doi.org/10.1111/jgh.15009.
- Nseir, William et al. 2010, “Soft drinks consumption and nonalcoholic fatty liver disease.” World Journal of Gastroenterology, vol. 16, no. 21, pp 2579-2588.