Blog
Food cravings and gut bugs
 You really want that doughnut/hot dog/bag o’ skittles. But you shouldn’t. But you really, REALLY want it.
You really want that doughnut/hot dog/bag o’ skittles. But you shouldn’t. But you really, REALLY want it.
You tell yourself, “Show some self-restraint!” or “Be ‘strong’ and resist!”.
Warring with ourselves over what we eat is not uncommon. However, it can be unhelpful. We need to learn to be kinder to ourselves, and not beat ourselves up when we eat or drink something not so great for us.
As it turns out, there are MANY factors that can influence food choice (it ain’t necessarily about willpower). And science suggests that the microbes of our intestinal microbiome may have a say in our desire for particular foods.
Food cravings and our gut bugs
There could be any number of reasons we crave something. Habit, low-energy, a hangover… but could it be, at least in part, particular gut bugs desiring particular nutrients from particular foods driving our food choices?
“Microbes have the capacity to manipulate behavior and mood through altering the neural signals in the vagus nerve, changing taste receptors, producing toxins to make us feel bad, and releasing chemical rewards to make us feel good,” said Athena Aktipis PhD, co-founder of the Center for Evolution and Cancer.
Aktipis and co-authors Carlo Maley and Joe Alcock published an interesting overview article in Bioessays, discussing several potential mechanisms that gut microbes could influence our eating behaviour.
This may include microbial production of mood-manipulating toxins; controlling the vagus nerve which is the highway between the gut and the brain; changing taste and other receptors and; influencing reward and satiety pathways.1
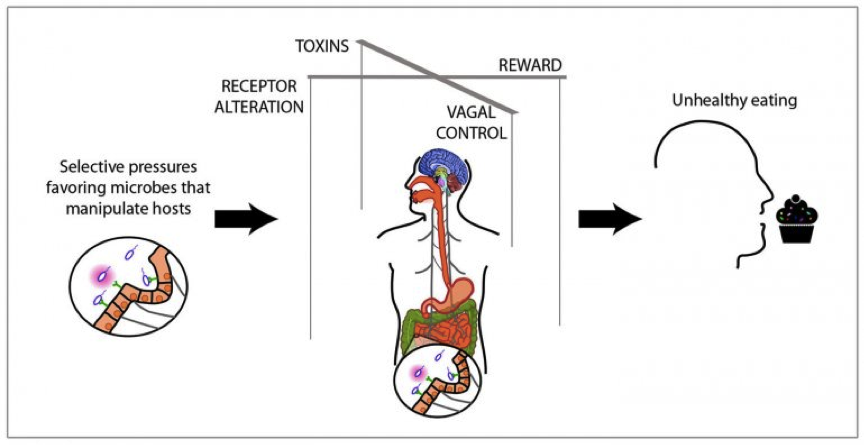
Whilst some microbes may influence food choice depending on their needs, it can work for or against us depending on what bugs predominate.
“Gut bacteria are manipulative,” says director of the UCSF Center for Evolution and Cancer, Carlo Maley. “There is a diversity of interests represented in the microbiome, some aligned with our own dietary goals, and others not.”
Sugar and gut bugs
The greatest concentration of intestinal microbes is in the colon. However, there are a few the reside in the small intestine.
Ideally, sugars we eat are consumed as part of a whole food usually alongside plant fibre. Fibre gets all the way to the colon to feed our helpful gut bugs.2
But simple sugars like those in added sugars and heavily refined and processed grains are rapidly absorbed in the small intestine, not reaching the colon. Instead these feed certain pathogenic, unhelpful bacteria. This can lead to their overgrowth and may contribute to a damaged intestinal lining, inflammation, gastrointestinal disorders, other symptoms systemically, and perhaps those sugar cravings in order to thrive.2-3
We still have a choice
Does this mean you are victim to a lifetime of scoffing a high added sugar foods like chocolate milk, low-fat strawberry flavoured yoghurt, soft drink and Ribena juice all day everyday because of gut bug desires?
Perhaps not.
Research has seen we can change the composition of our intestinal microbiome, though the speed in which this happens will vary across individuals. For a healthier microbiome, one will need to persist with a healthy diet over time for health changing effects.4
Fibre is important, including soluble, insoluble and resistant starch. Resistant starch specifically has been linked to increased insulin sensitivity, which may be due to keeping the right gut bugs fed and happy.5
A nutrient-dense, real food diet, that includes fibre and some fermented foods rich in probiotics, is thought to encourage microbial diversity, and diversity is associated with better health outcomes.
It has been hypothesised that the more diverse the microbial populations, the less opportunity for specific species to dominate and heavily influence how the host (i.e. you or I) eats or acts.1
Overall, when you do experience desire for food or drink you know aren’t particularly good for you, and you have it, don’t beat yourself up. Treats are okay. Enjoy it for what it is, and choose a super nourishing, gut bug friendly food or meal the next time you eat.
By Angela Johnson (BHSc Nut. Med)
References
- Alcock, J, Maley, CC, & Aktipis, CA 2014, ‘Is eating behavior manipulated by the gastrointestinal microbiota? Evolutionary pressures and potential mechanisms’, Bioessays: News And Reviews In Molecular, Cellular And Developmental Biology, vol. 36, no. 10, pp. 940-949.
- Baumler, AJ, & Sperandio, V 2016, ‘Interactions between the microbiota and pathogenic bacteria in the gut’, Nature, no. 7610, p. 85.
- Brown, K, DeCoffe, D, Molcan, E, & Gibson, DL 2012, ‘Diet-Induced Dysbiosis of the Intestinal Microbiota and the Effects on Immunity and Disease’, Nutrients, vol. 4, no. 8, pp. 1095-1119.
- Griffin, NW, Ahern, PP, Cheng, J, Heath, AC, Ilkayeva, O, Newgard, CB, Fontana, L, & Gordon, JI 2017, ‘Article: Prior Dietary Practices and Connections to a Human Gut Microbial Metacommunity Alter Responses to Diet Interventions’, Cell Host & Microbe, vol. 21, pp. 84-96.
- Johnston, KL, Thomas, EL, Bell, JD, Frost, GS, & Robertson, MD 2010, ‘Resistant starch improves insulin sensitivity in metabolic syndrome’, Diabetic Medicine: A Journal Of The British Diabetic Association, vol. 27, no. 4, pp. 391-397.











